A lot of exercise advice for people over 50 can be summarized in two words: “Just exercise.” And while exercise is certainly better than doing nothing (and it’s better to be fit than just active), that advice ignores something extremely important: The details of how you exercise make a huge difference in the results you get.
Exercise Prescription
When a doctor prescribes a medication, there’s a lot of precision behind it:
- Name of medication
- Dosage
- With food or away from food
- Morning or evening
Well, exercise is medicine too (in a very real sense, since it changes some health markers on par with, and in some cases, better than, the best medications out there), but like any medicine, the dosage determines whether it works.
Somehow, when exercise is prescribed, it changes from the same level of precision to a simple yes/no. Yes, you exercise or no, you don’t exercise. However, this is missing a lot of key details that make the difference between exercise that’s effective and exercise that’s ineffective. When it comes to strength training, the details that you need to know to make it effective for any goal are:
- Frequency: number of days per week
- Intensity: how much weight to lift/how much resistance to use
- Volume: number of sets and reps
- Structure: full body workouts or body part splits
- Exercise selection
For cardio, you need these details:
- Frequency
- Intensity: intensity is measured by your pulse.
- Duration
- Steady cardio or intervals
- If doing intervals, you also need to know:
- The number of intervals
- The duration of each interval
- The rest period between intervals
Why are these details important to know and follow? Because you want:
- Maximum effectiveness
- The best use of your time
Doing exercise the right way doesn’t take any more time than doing it the wrong way, but it makes all the difference as far as effectiveness is concerned.
Case in point:
Diabetes
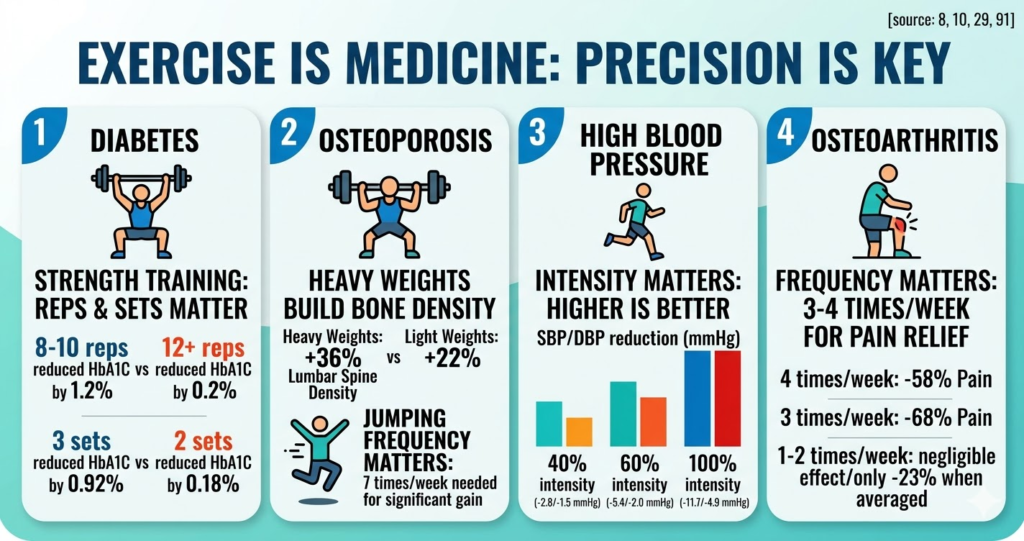
In my diabetes book, I prescribe 8-10 reps. That’s because in the study where people did 8-10 reps, HbA1C dropped by 1.2%, without any other changes (for non-diabetics, this doesn’t seem like much, so just for reference, the A1C of a diabetic is at least 6.5%. So a 1.2% drop is huge). Yet, another meta-analysis showed that when you start using weights light enough to allow you to do more than 12 reps, HbA1C is reduce by only about 0.2%. Even if you put a lot of effort into it, and get tired at the end.
The rep range also answers the question of weight selection. It’s not like you take a light weight that you can do 20 times, and stop at 10. That wouldn’t work. If you’re doing 8-10 reps, the weight needs to be heavy enough that you can lift it 9-12 times.
In other words, the difference between 8 reps and 15 reps can mean the difference between major metabolic improvement and barely any change.
There’s another big difference between the number of sets. In one meta-analysis, in diabetics who only did 2 sets per exercise, their HbA1C dropped by only 0.18%. In diabetics who did 3 sets per exercise, their HbA1C dropped by 0.92%. Slightly more work for five times better results.
That’s why when I talk to diabetic clients, and they say they’re strength training, I need to ask a lot of follow-up questions to see if they’re strength training effectively or ineffectively. You can see that the difference between doing it properly vs. improperly makes a huge difference to the bottom line.
This is just an example of strength training – but the same is true for cardio when it comes to type 2 diabetes. There’s an effective way to do it, and an ineffective way to do it. So it’s not just a binary yes/no (I do cardio or I don’t do cardio), but more like “how do you do cardio?”
Osteoporosis
In my osteoporosis book, I also prescribe relatively heavy weights. Why? Because as with diabetes, there’s a giant difference in bone density from training with heavy weights and training with light weights. In one study, women with osteoporosis were divided into 3 groups:
- Group 1: didn’t exercise
- Group 2: used light weights
- Group 3: used heavy weights
At the end of the study, here’s what happened to the bone density of the lumbar spine:
- Group 1 was unchanged
- Group 2 improved by 22%
- Group 3 improved by 36%
The implications of this are monumental. Group 2 would have to train for an extra 9-15 months to get to the same place that group 3 did in 6 months.
We also know that jumping is an effective way to improve bone density in people with osteoporosis. One study wanted to answer the question of “how much?” They divided people with osteoporosis into 4 groups:
- Group 1: didn’t jump
- Group 2: jumped twice per week
- Group 3: jumped 4 times per week
- Group 4: jumped 7 times per week
At the end of the study (6 months), the first 2 groups didn’t improve at all, and group 4 improved their bone density by 1.8% (a pretty impressive amount for 6 months).
So again, it changes the question from “are you jumping” to “how much are you jumping? How many days per week? How many jumps per workout? What’s the height of the jumps?” It’s those details that make the difference between effective jumping and ineffective jumping, as opposed to a binary jumping/not jumping.
High Blood Pressure
What was true for diabetes and osteoporosis is also true for high blood pressure. It’s the details that make the difference. As I talk about in my high blood pressure book, one study wanted to answer the question of optimal intensity. Is there an optimal intensity at which to exercise to lower blood pressure? Is it a “more is better” type of thing, or is there a point which is optimal? The short answer: it seems that yes, in this case, more is better. Here’s what they did:
They took 45 middle-aged, overweight men with blood pressures ranging from 120/80 (the average was 144.5/84.4 mmHg), up to 159/99, and poor cholesterol profiles. They were divided into 4 groups:
- Group 1 did nothing. They were the control group
- Group 2 exercised at 40% of their maximal aerobic capacity
- Group 3 exercised at 60% of their maximal aerobic capacity
- Group 4 went all out, and exercised at 100% of their maximal capacity
The results were:
- Group 2 reduced their systolic blood pressure by an average of 2.8 mmHg, and their diastolic blood pressure by 1.5 mmHg.
- Group 3 reduced their systolic blood pressure by an average of 5.4 mmHg, and their diastolic by 2.0 mmHg.
- Group 4 reduced their systolic blood pressure by an average of 11.7 mmHg, and their diastolic by 4.9 mmHg.
Osteoarthritis
In my arthritis book, I point out that exercise frequency also matters.
Another meta-analysis showed that doing strength training 4 times per week reduced pain by 58%, but 1-3 times per week reduced pain by 23%. In that meta-analysis, 1-3 times per week was grouped into one category. But from the previous meta-analysis, we saw that 1-2 times per week had negligible effects on strength, and yet, when a third day was added into the mix, it really skewed the average upwards – to 23%. So what kinds of pain reductions can be expected with 3 days per week?
One meta-analysis showed that strength training 3 times per week reduced pain by 68%, but twice per week only 41%.
The above are just a few illustrations of the need for specificity in exercise prescription. It’s not like one form of exercise is good for everything. What’s good for osteoporosis is not good for osteoarthritis. What works for diabetes may not necessarily work for high cholesterol. Hence why exercise prescription needs to given more attention than just the binary yes/no choice of do you exercise or not.
Why Most People Don’t Know Exercise Prescription
If these tiny changes make big differences in terms of effectiveness, why isn’t this more common knowledge among health professionals?
- Exercise programming is not in the domain of doctors. They get almost no training on exercise prescription, other than “exercise is good for you.”
- Physical therapists deal more often with acute injuries, as opposed to chronic conditions. And even then, many of them use modalities (lasers, hot packs, cold packs, acupuncture, etc.), and exercise is often an afterthought.
- Personal trainers and kinesiologists aren’t taught exercise programming for chronic conditions – just programming for the general public. I have both a kinesiology degree, and have had multiple personal training certifications over the years, and none of this stuff was taught to me in my degree or certifications.
The examples above illustrate an important point: exercise is not just about doing something. The details matter. The number of sets, the rep range, the weight used, the frequency of training, the intensity of cardio, etc.
Small changes in these variables can produce dramatically different results, even when the exercises themselves look almost identical.
Want to Know If Your Exercise Program Is Actually Working?
Many of the people who come to see us are already exercising.
But once we look at their program, we often find small details that are holding back their results.
Things like:
- The wrong rep range
• Too few sets
• Insufficient intensity
• The wrong exercise selection
Fixing those details can dramatically improve the results they get.
If you’d like us to take a look at your current exercise program, or build a brand new one for you, you can see whether you qualify for our services by just filling out the application form on our home page. Doing so doesn’t obligate you to anything. It simply sets up a quick, 10-15-minute chat where we’ll discuss your current situation, and see whether we can work together. There’s no sales pitch, obligation or pressure.

